Failing to address the scourge of antibiotic-resistant bacteria will deny patients the benefits of scientific advancements and threaten thousands of lives, a new study from the Center for Disease, Dynamics, Economics & Policy suggests.
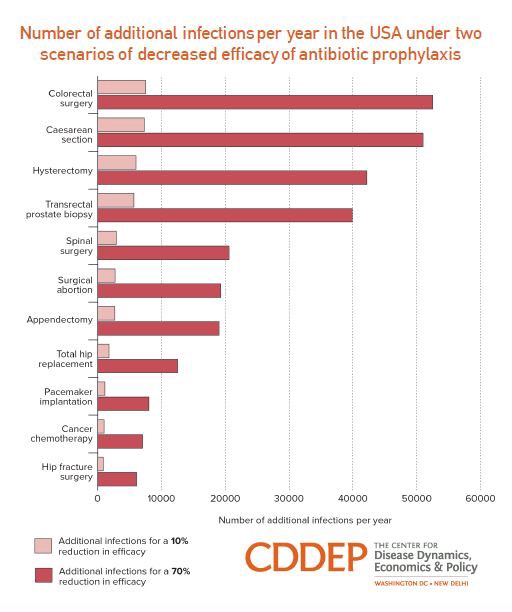
The recent study, published in the latest issue of the medical journal The Lancet, predicts nearly 120,000 infections and 6,000 deaths over a seven-year span in a scenario in which antibiotic effectiveness falls by 30 percent. To reach this conclusion, researchers analyzed the findings of hundreds of clinical trials, involving the 10 most common surgical procedures, and calculated trends in antibiotic potency over the past seven years.
The report acknowledges the need for more data to establish clear recommendations to prevent this scenario. But lead researcher Ramanan Laxminarayan said his findings do show that time is of the essence when it comes to spreading awareness about the dangers of antibiotic misuse in the medical industry — designated as a key cause of antibiotic resistance.
This is a serious threat that the Centers for Disease Control and Prevention (CDC) describes as a nightmare.
“We need to change the way people see antibiotics,” Laxminarayan, also a member of the Presidential Advisory Council on Combating Antibiotic Resistant Bacteria, told ThinkProgress.
Last year, the White House formed a task force to develop a five-year plan to prevent the rise of antibiotic resistance. President Barack Obama also announced that federal cafeterias would start purchasing beef and poultry with lower quantities of antibiotics. If the federal government continues along this course, it will follow in the footsteps of Sweden, which curbed antibiotic use by 40 percent in the mid-1990s.
“There has been amazing progress on President Obama’s part but we need to see action and money from Congress,” Laxminarayan said. “This is a serious threat that the Centers for Disease Control and Prevention (CDC) describes as a nightmare. We have the opportunity to handle this now.”
“The cost of dealing with this late would be much greater,” he added.
While antibiotics — synthetic compounds that kill microorganisms — have been effective in the past, research has found that when patients don’t take their medication as prescribed or doctors dole out huge amounts, they don’t work beyond the suggested timespan. Common ailments for which practitioners overuse antibiotics include mild sinusitis, the common cold, and eye and ear infections, according to data compiled by the American Academy of Family Physicians and the American Academy of Pediatrics.
When antibiotics don’t work as intended, bacteria isn’t wiped out in its entirety, eventually developing into a stronger, drug-resistant form. Nearly 23,000 people die annually and nearly 2 million become sick because of improper antibiotic use, according to the CDC. Other effects include prolonged hospitalization, additional tests, lost income, and higher medical costs.
“There has sort of been a longstanding idea that because antibiotics were so cheap, you could give it to someone who wasn’t feeling so well,” Laxminarayan said. “If they didn’t know what was happening with the patient, they used antibiotics but they didn’t feel any better.”
Changing minds about antibiotic use could prove to be a huge undertaking.
Despite the fact that 90 percent of health professionals have some awareness about antibiotic resistance, few in the medical field believe the onus is on them to cut down their use. A recent review of scientific studies showed that members of this group instead blame other doctors, people who overuse their medication, and even the government for not tackling the issue. Some respondents also said they didn’t see antibiotic resistance as a priority when treating individual patients, choosing instead to pass that responsibility on to other parties.
All of the things we consider modern medicine depend on antibiotics. Without them, these infections could lead to death.
However, the effects of that lackadaisical attitude go beyond the United States. A British-commissioned review released last year showed that, if left unabated, drug-resistant superbugs could kill an additional 10 million people annually and drive health care costs up by $100 million by 2050. The study followed warnings from global health officials — including World Health Organization head Margaret Chan and English Chief Medical Officer Dame Sally Davies — about the link between antibiotic overuse and rise of this new class of superbugs.
“Antibiotic resistance is a direct threat to the well-being of ordinary people who need to depend on antibiotics to treat everyday infections,” infectious disease specialist Dr. Timothy Leahy told ThinkProgress last year. “There are only two ways to fight antibiotic resistance: stop antibiotic misuse and create new antibiotics. Both are challenging because they require us to balance public health concerns with either ingrained habits or vested interests.”
Scientists at the University of York in the United Kingdom have taken those steps recently, mixing and matching the genes from different antibiotic biosynthesis pathways to create new antibiotics. This process goes beyond that used to produce its predecessors. The group said their findings, outlined in a study, could also lead to the improvement of existing antibiotics.
Even so, Laxminarayan says a reduction in the use of antibiotics should remain a key strategy in making diseases less resistant. According to him, that requires challenging the mindset that the emergence of superbugs isn’t any cause for worry.
“Most folks forget that someone will need surgery at one point, whether it’s a C-section, knee replacement, or biopsy. All of the things we consider modern medicine depend on antibiotics. Without them, these infections could lead to death,” he said.
