On Tuesday, the World Health Organization announced the end of the most recent Ebola outbreak in the Democratic Republic of Congo, which infected dozens of people and killed 33 between early May and July of this year.
“The outbreak was contained due to the tireless efforts of local teams, the support of partners, the generosity of donors, and the effective leadership of the Ministry of Health. That kind of leadership, allied with strong collaboration between partners, saves lives,” WHO Director-General Dr. Tedros Adhanom Ghebreyesus said in a press release.
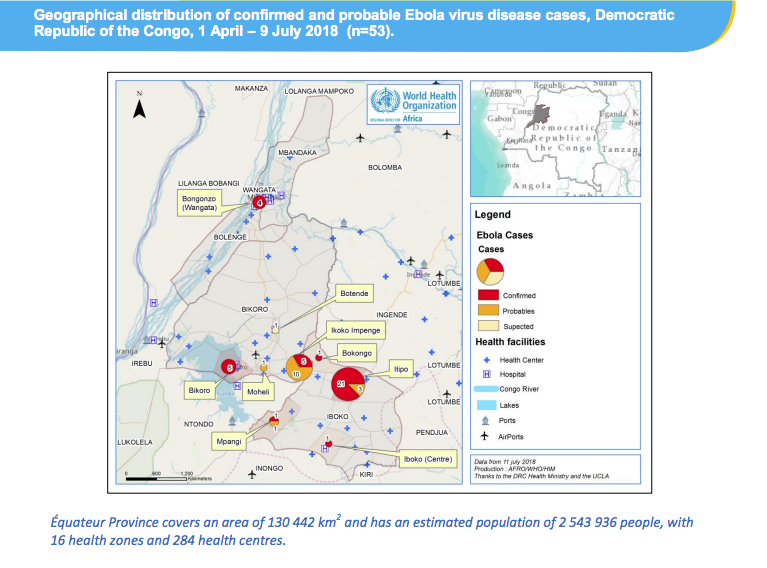
The DRC Ebola Virus disease (EVD) outbreak was first declared on May 8 in the Bikoro health zone and later spread to the Iboko and Wangata health zones. It remained relatively isolated there until May 18, when officials announced the virus had reached the port city of Mbandaka, a major economic hub of around 1.2 million people that sits directly along the Congo River. On May 21, health officials said two infected individuals had escaped a treatment facility inside Mbandaka, complicating things further. Both patients died within the day, one at their home and the other at the treatment facility, after returning to the premises.
GREAT NEWS! The most recent #Ebola outbreak in the Democratic Republic of the Congo is now officially over.
WHO calls for international efforts to stop other deadly outbreaks in #DRC 🇨🇩
More info 📰: https://t.co/goXhK9Rijr #alert pic.twitter.com/QXZYHmOSmR
— World Health Organization (WHO) (@WHO) July 24, 2018
The rapidly spreading outbreak brought to mind memories of the 2014 West Africa outbreak, which killed 11,000 people as it spread across Guinea, Sierra Leone, Liberia, Nigeria, and Mali. A handful of western nations, including the United States, also saw a number of isolated cases, prompting a revived sense of urgency behind the development of a vaccine.
In the years that followed, researchers went to work developing the VSV-ZEBOV Ebola vaccine, known as V920. After several successful human trials, researchers debuted the Merck-manufactured vaccine in late 2016, and in May this year, WHO and regional health workers tapped into the existing stockpile to begin ring-vaccinations to limit the spread of the DRC outbreak.
“WHO moved quickly and efficiently,” WHO Regional Director for Africa Dr. Matshidiso Moeti stated Tuesday. “We also demonstrated the tremendous capacity of the African region. More than three-quarters of the 360 people deployed to respond came from within the region. Dozens of experts from Guinea spent weeks leading Ebola vaccination efforts here, transferring expertise which will enable the DRC to mount an effective response both within its borders and beyond.”
Health workers ultimately administered the V920 vaccine to nearly 7,000 people across four health zones, all of whom may have potentially had contact with the infected. The vaccine — and the health workers’ rapid response — appears to have slowed the outbreak significantly.
Early global response to the outbreak also limited its reach. WHO officials on Tuesday recognized several nations for their financial contributions to the response effort, including Germany, whose contribution will “go to replenish the CFE [Contingency Fund for Emergencies],” which provided initial monetary assistance.
Officials also noted the contributions of nations like Norway, which provided in-kind contributions for medical evaluation, and EU ECHO — European civil protection and humanitarian aid operations — for providing flights between Mbandaka and Kinshasa, where the National Institute of Biomedical Research is located. Guinea, the United Kingdom, Germany, and the United States also provided technical assistance.
Although the DRC outbreak is officially over, STAT notes a new paper published by The Lancet on Tuesday has triggered alarm bells for health workers monitoring its aftermath.
According to researchers, health workers identified an EVD cluster in Liberia in 2015, long after a past outbreak in the region had been declared over, which included three infected individuals: an infected 15-year-old boy, his brother, and his father. The infections appeared to be phylogenetically related to a similar outbreak in the region from August 2014.
Researchers concluded that the boys’ mother had become infected during the August 2014 outbreak but was never diagnosed, and that she had inadvertently spread the virus to her family after living with it, unaware, for a year.
“Based on serology and epidemiological and genomic data, the most plausible scenario is that a female case in the November, 2015, cluster survived Ebola virus disease in 2014, had viral persistence or recurrent disease, and transmitted the virus to three family members a year later,” they wrote.
The idea of extended viral persistence not only signals a potential longterm health crisis, but adds to the stigma many Ebola patients already face, STAT’s Megan Thielking noted.
“Viral persistence has been seen before — but up until now, most transmission has been from men to women through semen,” she wrote. “The authors say survivors can trigger resurgence of Ebola’s spread in some cases, which experts warn could increase the substantial stigma that Ebola survivors can face.”
Researchers warned that the case presents added pressure for regional health workers to keep a closer eye on patients and their contacts, in order to prevent future epidemics.
“Investigation of the source of infection for the November 2015, cluster provides evidence of Ebola virus persistence and highlights the risk for outbreaks after interruption of active transmission,” they wrote. “These findings underscore the need for focused prevention efforts among survivors and sustained capacity to rapidly detect and respond to new Ebola virus disease cases to prevent recurrence of a widespread outbreak.”
Correction: An earlier version of this article stated the death toll from the DRC Ebola outbreak was 29. It has been corrected with the most recent information to reflect the fact that 33 people were killed.

